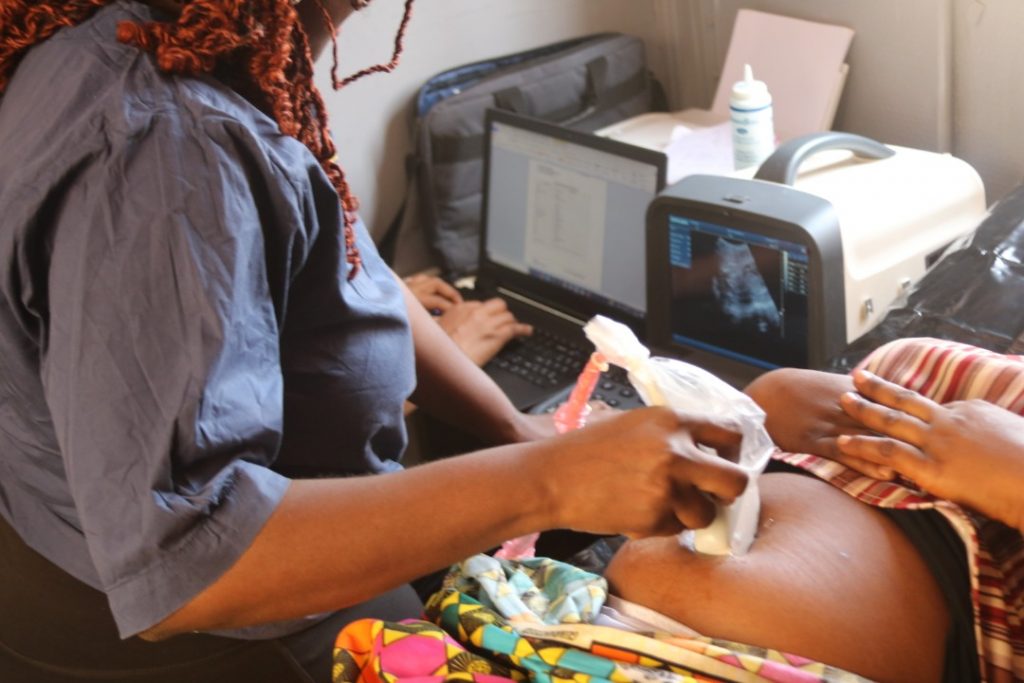
A number of pregnancies (27 percent) are affected by a chronic condition (Statistics Canada, 2018). When diagnosis of a birth defect is necessary, ultrasounds help guide the more invasive diagnostic tests of amniocentesis and chorionic villus sampling. Amniocentesis is a procedure in which a needle is used to withdraw a small amount of amniotic fluid and cells from the sac surrounding the fetus and later tested. Chorionic villus sampling is a procedure in which a small sample of cells is taken from the placenta and tested. Both amniocentesis and chorionic villus sampling have a risk of miscarriage, and consequently they are not done routinely.
Box 2.4: Infertility and Reproductive TechnologyInfertility: Infertility affects about 16 percent of couples in Canada (Canada, 2019). This number has doubled since the 1980s. Male factors create infertility in about a third of the cases. For men, the most common cause is a lack of sperm production or low sperm production. Female factors cause infertility in another third of cases. For women, one of the most common causes of infertility is the failure to ovulate. Another cause of infertility in women is pelvic inflammatory disease (PID), which is an infection of a woman’s reproductive organs (Carroll, 2007). It is a complication often caused by some STDs, such as chlamydia and gonorrhea. Other infections that are not sexually transmitted can also cause PID. There are approximately 100,000 cases of symptomatic PID annually in Canada. Based on a nationally representative sample from 2006-2010, 5 percent of US women have reported being treated for PID in their lifetime, and 1 in 8 women with a history of PID experience difficulties getting pregnant (CDC, 2014). Both male and female factors contribute to the remainder of cases of infertility. Fertility treatment: The majority of infertility cases are treated using fertility drugs to increase ovulation or with surgical procedures to repair the reproductive organs or remove scar tissue from the reproductive tract. In vitro fertilization (IVF) is used when a woman has blocked or deformed fallopian tubes or sometimes when a man has a very low sperm count. This procedure involves removing eggs from the female and fertilizing the eggs outside the woman’s body. The fertilized egg is then reinserted in the woman’s uterus. The average costs of IVF are between $7,750 and $12,250. Medication alone can cost anywhere from $2,500 to $7,000. The success rate varies depending on the age of the mother and type of egg implanted, such as whether the egg was recently removed from the woman, used after being frozen, or donated from another woman. According to a 2006 CDC report on assisted reproductive technologies that led to a healthy baby, the percentages were as follows:
Higher success rates, but less common procedures include gamete intra-fallopian tube transfer (GIFT) which involves implanting both sperm and ova into the fallopian tube and fertilization is allowed to occur naturally (Carroll, 2007). Zygote intra-fallopian tube transfer (ZIFT) is another procedure in which sperm and ova are fertilized outside of the woman’s body and the fertilized egg or zygote is then implanted in the fallopian tube. This allows the zygote to travel down the fallopian tube and embed in the lining of the uterus naturally. This procedure also has a higher success rate than IVF. The Assisted Human Reproduction Act is a law enacted by the Parliament of Canada in 2007. Its purpose is to regulate assisted human reproduction (AHR) and related research. It is one of the most comprehensive pieces of legislation in the world concerning reproductive technologies and related research. The AHR Act was meant to provide Canadians with a system of licensing, monitoring, inspection, and enforcement of activities relating to AHR in order to protect and promote Canadians’ health, safety, and values. A 2010 Supreme Court case that ruled that certain sections of the AHR Act exceeded the federal government’s legislative power means that the scope of the AHR Act’s regulatory framework was significantly reduced (for sections 10,11,13, 14-18, 40(2), 40(3), 40(3.1), 40(4), 40(5), 44(2), and 44(3)). |

